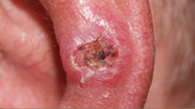
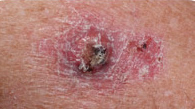
Squamous Cell Carcinoma
Squamous cell carcinoma is the second most common form of skin cancer, affecting more than 250,000 Americans a year. If left untreated, squamous cell carcinoma has the potential to spread to other areas of the body and become life-threatening.
Like other forms of skin cancer, squamous cell carcinoma is most common in areas of the body that are frequently exposed to the sun. However, this type of tumor can occur on other parts of the body as well.
Warning signs include a wart-like growth or a scaly red patch, an open, non-healing sore, or an elevated growth. These lesions can occasionally bleed or crust over and may have borders that are difficult to define.
Actinic keratoses can be pre-cursors of squamous cell carcinoma, frequently occurring on the face, exposed areas of the scalp, torso and extremities. People with fair skin and light colored hair and eyes have an increased risk of developing squamous cell carcinoma. In addition, patients whose immune systems are compromised, such as organ-transplant patients on immunosuppressive medication, are at an increased risk of developing squamous cell carcinoma.
A biopsy is required to confirmed a diagnosis. An early, superficial form of squamous cell carcinoma is squamous cell carcinoma in-situ. In-situ involves the outer surface of the skin only, and has not yet developed an invasive component.
Specialties
- Agnes RF
- Blue Light & Levulan
- Botox Cosmetic
- Cellulaze
- Chemical Peels
- Clear + Brilliant Laser
- CoolSclupting
- CoolTone
- Cosmopen
- DAXXIFY
- Dermal Fillers
- Elite Laser
- FotoFacial
- Fraxel Dual Laser
- FX Laser Resurfacing
- HydraFacial
- Kybella
- Latisse for Lashes
- Laser Hair Removal
- MiraDry
- PicoSure Laser
- PRP Hair Restoration
- Scarlet SRF
- Scar Revision
- Sclerotherapy
- Skin Cancer Reconstruction
- SmartLipo
- SofTap
- Tattoo Removal
- Ultherapy
Treatment
Curettage and Electrodesiccation
This procedure is typically limited to the treatment of squamous cell carcinoma in situ. This procedure uses a surgical instrument (curette) to scrape the cancer cells away from the skin surface, followed by burning the skin surface with an electric needle. The wound is allowed to heal without suturing. This procedure has a cure rate of 90%. One disadvantage of this procedure is that it may result in a whitish scar which may be depressed.
Radiation
Radiation is an effective treatment for squamous cell skin cancer, with a cure rate of approximately 90%. One advantage of radiation treatment is the avoidance of a surgical procedure. Disadvantages of radiation include the need for a series of treatments over a several week period. In addition, the skin may develop radiation changes (loss of pigmentation and a shiny appearance). These changes may occur several years after the radiation is completed. Radiation is often recommended for patients who are suboptimal surgical candidates.
Excisional Surgery
This involves the surgical removal of the tumor using local anesthesia and closure of the wound with sutures. The excised specimen is submitted for pathology processing to be certain that the cancer is completely removed. The pathology results typically take several days to become available. The cure rate with this procedure is approximately 90%.
Excisional Surgery with Conventional Frozen Section Margin Control
This procedure, which is often performed in a hospital setting, involves checking the pathology with conventional (non-Mohs) frozen sections prior to closing the surgical wound. If tumor extends to the edges of the specimen, additional tissue is removed prior to closing the wound. This method does not examine 100% of the surgical margins, and thus the potential exists for cancer cells to be undetected at the wound edges. Conventional frozen section margin control provides a cure rate of approximately 95%.
Mohs Micrographic Surgery
Mohs micrographic surgery provides the highest possible cure rate of all treatments for squamous cell carcinoma, with a cure rate of greater than 98% for previously untreated tumors. The procedure is performed in the office using local anesthesia. With Mohs micrographic surgery, the pathology is processed using frozen sections prior to closing the wound. If the tumor extends to the wound edges, an additional layer of tissue is removed and processed. The tissue processing with Mohs Surgery is more thorough than conventional frozen section margin control. With Mohs, 100% of the surgical margins are assessed, which accounts for the higher cure rate with Mohs surgery. Mohs surgery also preserves the greatest amount of healthy skin, resulting in the smallest possible surgical defect. One disadvantage of Mohs Micrographic surgery is the potential length of the procedure, which may take several hours to complete.